Necrotic enteritis is a bacterial digestive disease common in chicken and turkey farming. While the etiopathogenesis of the agent is well known, the triggering factors are still being discussed. However, the resurgence of this disease has coincided with changes in poultry feed. In addition to clinical consequences (mortality), the disease also has important economic consequences : additional drug costs, zootechnical underperformance, increased seizures in slaughterhouses.
The disease agent and its pathogenicity
- The agent responsible for this disease is Clostridium perfringens (type A or C). It is a common bacterium, often found in the environment in rotting materials, and is also a normal host of the digestive tract. It is a strict anaerobic anaerobic sporulated Gram positive bacillus.
- C. perfringens type A produces alpha toxin, and some strains also produce an enterotoxin synthesized during sporulation. The virulence of these A strains is variable.
- In addition to necrotic enteritis, C. perfringens can be responsible for gizzard erosions and gangrenous dermatitis in birds, among other things.
- Under good conditions, the population of this bacterium grows rapidly, it doubles in 3-5 minutes. This explains the suddenness of Clostridium infections and the need to react quickly.
- The spore is resistant to heat (100-120°C), oxygen, drought, so it resists well in outdoor environments.
Epidemiological data
Necrotic enteritis mainly affects chickens and turkeys, between 2 and 5 weeks of age. High quality chickens (“Poulet label” in France) and pullets can also be sick.
The germ enters poultry by the oral route. It is carried by soiled litter, animal excreta, food. There is no direct contact transmission. Vectorized (flies) or vertical transmissions are also suspected.
Clostridia remain in the flow of the digestive content, they do not attach to the digestive walls. Generally, ingestion does not cause anything. For disease to occur, several risk factors must occur simultaneously, and the concentration of bacteria must be very high to cause damage (1 million bacteria per g of digestive content). The disease is linked to the production of toxins responsible for intestinal wall necrosis and mortality.
It should be noted that certain types of foods seem to favour the development of clostridia : foods based on wheat or barley or sugars and proteins quickly available for the small intestine. For example, the prevalence of necrotic enteritis is 6 to 10 times higher in herds fed with wheat/barley feed compared to herds fed mainly with corn.
The zoonotic risk in the form of foodborne illness should not be neglected. It is linked to enterotoxins produced during sporulation. For example, poultry based food can cause disease in humans (diarrhea for type A, necrotic enteritis for type C).
There is also a subclinical form of the disease, caused by dysbacteriosis. Dysbacteriosis is defined as the presence of abnormal small intestinal flora in both quantity and quality. This imbalance of the digestive flora allows the implantation of C. perfringens.
C. perfringens plays a role in dysbacteriosis but it is not the only determining factor and it is not always involved. This form is under-diagnosed and is most common in 21-day-old broilers.
Clinical manifestations of the disease
- Necrotic enteritis is an acute disease with very rapid progression. 24 hours before, it is possible to observe an increase in water consumption. Then, the signs are prostration with ruffled feathers, anorexia, sometimes diarrhea. Affected individuals are often well conformed. Mortality can quickly reach 1-2% per day (with up to 50% cumulative mortality).
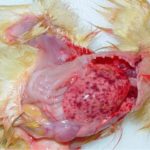
- Dead bodies putrefy quickly, especially the intestine. The contents of the small intestine are dilated by gas and take on a “bread crumb” appearance. The lesions are mainly localized in the jejunum and ileum. It begins with thickening and an opacity of the wall, with formation of fibrinonecrotic exudate. The intestine becomes dilated by a liquid and foul-smelling greenish content. The intestinal wall is brittle. Petechiae can also be observed.
- The liver may sometimes show discoloration and foci of necrosis.
- Necrotic enteritis also leads to zootechnical underperformance and increased seizures at the slaughterhouse.
- Subclinical form : no particular signs except diarrhea. The ratio of water consumed to food consumed and the CI are increased. This is the cause of poor zootechnical performance. The digestive villi are slightly abraded.
The diagnosis
Epidemio-clinical diagnosis
Acute disease with prostration, cessation of consumption, mortality, preceded by an increase in water consumption, “bread crumb” lesion, rapid putrefaction, repeated antibiotic treatments, contaminated site.
Differential diagnosis
Coccidiosis
Bacteriological diagnosis
With antibiotic susceptibility test
Disease prevention and control
Treatment
If the diagnosis is made quickly, the clinic can be managed with antibiotics. C. perfringens has a good sensitivity to certain antibiotics such as beta-lactam antibiotics and macrolides. Parasitic conditions should also be treated with anticoccidial agents (coccidiosis establishes a favourable breeding ground for clostridiosis).
Dans les élevages à entérite nécrotique chronique, pour lesquels les traitements ne sont plus efficaces bande après bande, il faut réaliser un audit, en focalisant notamment sur les pratiques d’hygiène (désinfection, sol, qualité de l’eau,…) et la conduite d’élevage.
Prevention
Monitoring water consumption : Daily monitoring of water consumption is a good preventive tool, because almost every time, an increase in water consumption precedes of 24-hour the appearance of mortality.
Hygiene and anti-parasite : The best prevention is hygiene in livestock farming : use of disinfectants registered at sporicidal doses, decontamination of water pipes (alkaline detergent and then acidic descaler), chlorination or even acidification of water, cleaning and disinfection of silos, decontamination of soils and around livestock sheds (quicklime 0.5kg/m3, caustic soda 0.1kg/m3). An effective (ionophore) and controlled anticoccidial program can also be useful during critical periods of the animal.
The case of Clostridium colinum
Clostridium colinum is the agent of ulcerative enteritis, which affects mainly quail but also sometimes young chickens, turkeys and game birds. It does not cause toxi-infections in humans. At the lesional level, ulcers of the intestinal mucosa are observed which can perforate and cause peritonitis. The liver may have yellowish to greyish lesions surrounded by a halo. The spleen is enlarged and hemorrhagic.